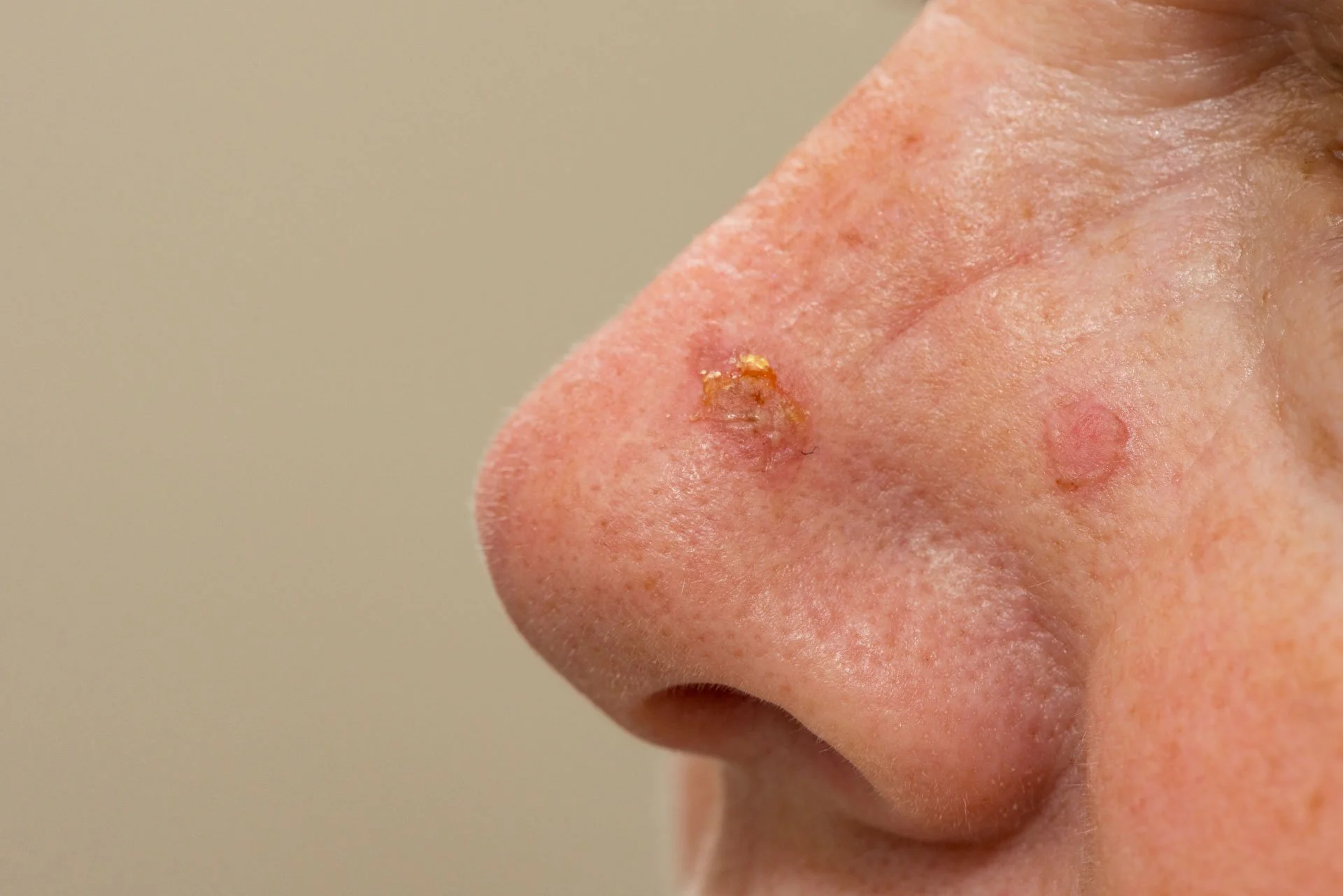
Focal photodynamic therapy for superficial skin cancers
Understanding focal PDT and who it suits
Photodynamic therapy uses a prescription light-activated medicine applied to the skin, then activated with a controlled light exposure. Once activated, it targets abnormal cells while preserving more normal surrounding tissue.
Intraepidermal carcinoma is an early form of squamous cell carcinoma confined to the top layer of skin. Superficial basal cell carcinoma is a type of BCC that tends to spread across the surface rather than grow deeply. These are the types of lesions where PDT can be a sensible option in carefully selected cases.
PDT is not suitable for every skin cancer. Thicker, aggressive, recurrent lesions, or lesions in higher-risk sites often require surgery. The first step is always confirming diagnosis and suitability.
At a glance

Treatment
Focal photodynamic therapy with LaseMD assisted medication delivery

Downtime
1-2 days downtime
7-10 days healing

Costs
From $1,495 per session

Approach
Confirm suitability, then treat focally with close follow up

Concern
Biopsy-proven intraepidermal carcinoma and selected superficial BCC

Course
2 Sessions, usually 6 weeks apart
Dr Mitch’s Take
When a biopsy confirms a superficial skin cancer, the next question is usually, “Do I need it cut out?” Sometimes the answer is yes. But for the right lesion, in the right spot, there are non-surgical options that can clear the cancer while keeping scarring and downtime to a minimum.
At DERM Skin Specialists, I use focal photodynamic therapy for biopsy-proven intraepidermal carcinoma, also called Bowen’s disease, and selected superficial basal cell carcinomas. In many cases, I use a LaseMD-assisted approach first to improve medication penetration before the activation step. The point is simple: treat precisely, heal well, and keep follow-up tight so we can be confident in the outcome.

What the journey looks like at
Derm Skin Specialists
01
Expert dermatologist review
A dermatologist reviews your biopsy result and confirms that the lesion type and location are suitable for focal PDT.
02
Personalised treatment plan
Your treatment is planned around your diagnosis, with clear advice on aftercare and expected downtime.
03
Treatment & follow-up
You’ll receive two treatment sessions, usually six weeks apart, followed by a review to assess response and agree on next steps.
How focal PDT is delivered
On the day, the area is cleaned and prepared. In selected cases, a short fractional LaseMD pass is performed first to assist absorption of the light-activated medicine into the target area. The medicine is then applied and allowed to incubate.
After a defined incubation period, the lesion is treated with the activation step. Most patients describe a warm, stinging sensation during activation. We manage comfort carefully and adjust technique depending on the site and the size of the treatment area.
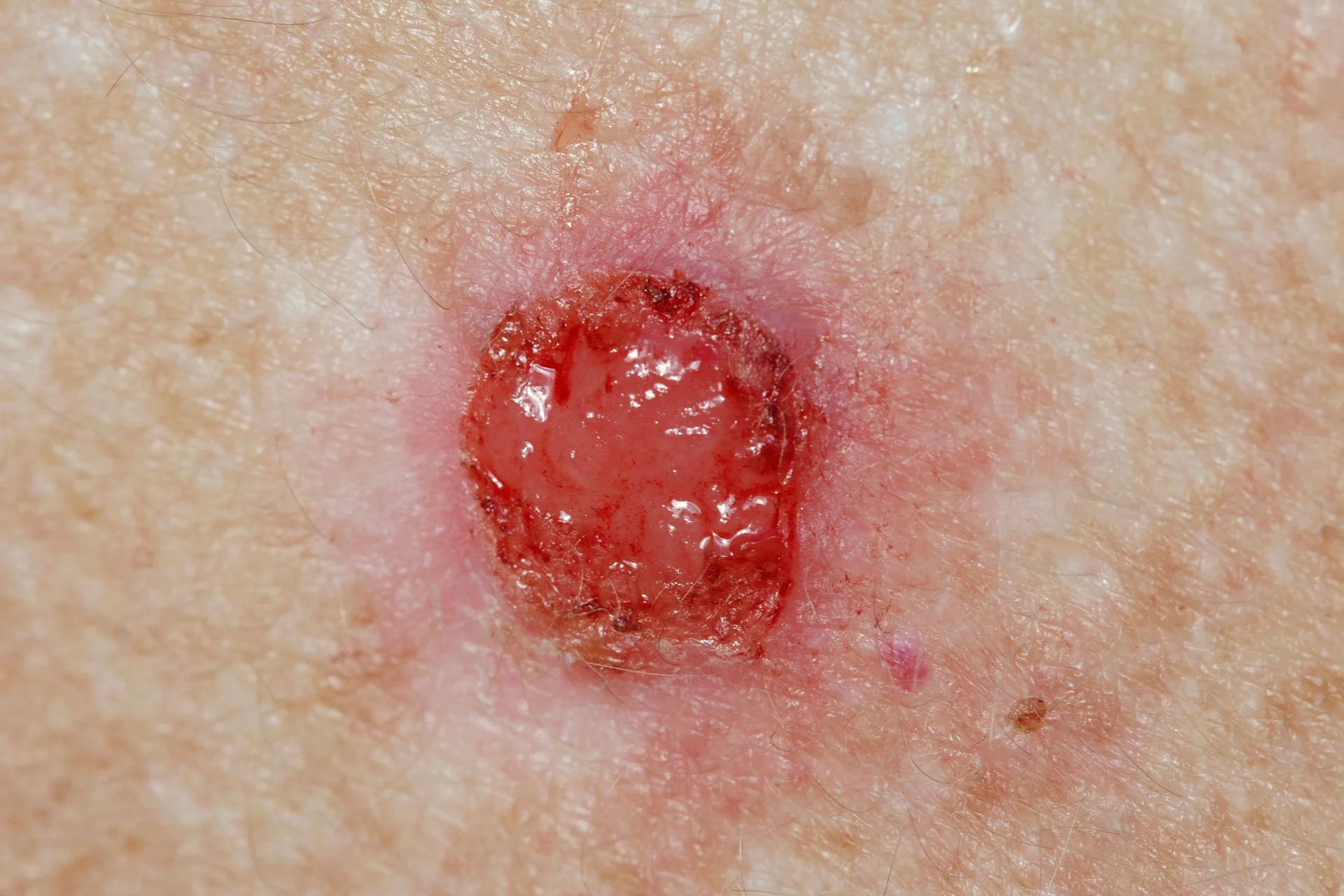
After treatment, the skin is expected to be inflamed. The area typically looks pink to red, then crusts or peels as healing progresses.
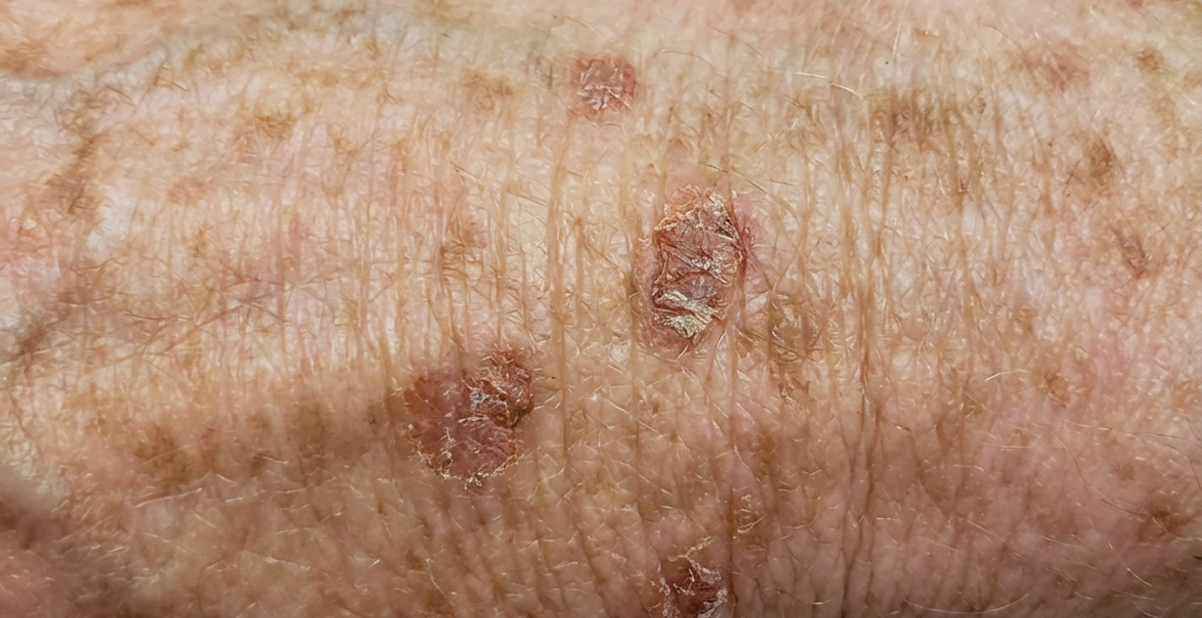
What results to expect
Medical disclaimer
This page is general information only. Suitability, expected outcomes and Medicare eligibility depends on individual assessment.
-
Focal PDT is an effective option for selected superficial skin cancers when the diagnosis and lesion type are right. Our aim is clearance with a tissue-sparing approach, then structured follow-up to confirm the response.
-
No skin cancer treatment is completely “set and forget”. Even when a lesion is surgically removed, there is still a small risk it can recur. That’s why we recommend ongoing monitoring whether you choose PDT or surgery.
-
Published clearance rates for PDT in suitable superficial lesions are commonly quoted in the 80–90% range. Surgical excision with appropriate margins generally has a higher clearance rate, often quoted around the mid-90% range, depending on the lesion type and site. That difference is exactly why we select cases carefully and build follow-up into the plan, whichever pathway you choose.
-
Downtime is typically 4 to 5 days. Expect redness, swelling, and some crusting or peeling.
Less common risks include infection, prolonged redness, pigment change, scarring, or incomplete clearance. Even with careful selection and good technique, recurrence can occur, which is why follow-up matters.
LaseMD field therapy at
Derm Skin Specialists
LaseMD is used for patients with broader sun damage and field change, especially when the pattern is recurring roughness in the same zone rather than a single isolated spot.

Typical Course
2 sessions, 6 weeks apart

Costs
$1,495 per session

Downtime
4-5 days of redness & flaking

Appointment Length
Approx 15 minutes
Not sure where to start?
If you have a biopsy result showing intraepidermal carcinoma or superficial basal cell carcinoma, the best next step is a dermatologist consultation at DERM Skin Specialists. That visit is where we confirm suitability, talk through options, and map out the safest plan.
Our Most Commonly Asked Questions
Medical disclaimer
This page is general information only. Suitability, expected outcomes and Medicare eligibility depends on individual assessment.
-
PDT is a non-surgical treatment where a light-activated medicine is applied to the lesion, then activated with a controlled light. It can be suitable for selected superficial cancers.
-
Yes, Photodynamic Therapy (PDT) can be an effective treatment option for superficial basal cell carcinoma (sBCC) in suitable cases. PDT uses a light-sensitive cream and a specialised light source to target and destroy abnormal skin cells.
PDT is generally best suited to superficial, low-risk lesions and areas where minimising scarring is preferred. It may not be suitable for deeper or more aggressive skin cancers.
A consultation with one of our clinicians is required to determine whether PDT is appropriate for your lesion.
-
Yes, Photodynamic Therapy (PDT) is commonly used to treat intraepidermal carcinoma (IEC), also known as Bowen’s Disease. PDT targets abnormal cells within the upper layers of the skin using a light-sensitive cream and specialised light source.
It can be an effective option for suitable lesions, particularly in areas where cosmetic outcome is important. A consultation is required to assess whether PDT is the most appropriate treatment for your skin.
-
Most patients experience some discomfort during Photodynamic Therapy (PDT), commonly described as a burning, stinging, prickling, or warm sensation while the light is active. The level of discomfort varies depending on the treatment area and individual sensitivity.
Any discomfort usually settles shortly after treatment, and your clinician can discuss ways to help make the procedure more comfortable.
-
ALA-PDT stands for Aminolevulinic Acid Photodynamic Therapy. It is a treatment that uses a light-sensitive solution called aminolevulinic acid (ALA) together with a specialised light source to target abnormal or damaged skin cells.
After the ALA is applied to the skin, it is absorbed by abnormal cells. The area is then exposed to light, which activates the solution and destroys the targeted cells while minimising damage to surrounding healthy tissue.
ALA-PDT is commonly used for certain sun-damaged skin conditions and superficial skin cancers.
-
Laser-assisted PDT is a technique where a laser is used before Photodynamic Therapy (PDT) to create tiny channels in the skin. This helps the light-sensitive solution penetrate more effectively into the treatment area.
By improving absorption, laser-assisted PDT may enhance treatment results for certain skin conditions and lesions. Your clinician will advise whether this approach is suitable for your skin and treatment goals.
-
The number of Photodynamic Therapy (PDT) sessions required depends on the condition being treated, the size and location of the area, and how your skin responds to treatment.
Some patients may achieve good results with a single session, while others may require a series of treatments for optimal outcomes. Your clinician will recommend a personalised treatment plan during your consultation.
-
After Photodynamic Therapy (PDT), it is common to experience redness, swelling, sensitivity, peeling, or crusting in the treated area. Downtime can vary depending on the treatment intensity and the area treated, but most patients experience visible skin reactions for around 5–10 days.
You will also need to avoid sun exposure immediately after treatment, as the skin will be highly light-sensitive. Your clinician will provide detailed aftercare instructions to support healing and recovery.
-
Photodynamic Therapy (PDT) can be an effective treatment for certain superficial skin cancers and precancerous lesions, however no treatment can guarantee that a lesion will not recur in the future.
Regular skin checks and ongoing monitoring are important after treatment, as some lesions may return or new skin cancers may develop over time. Your clinician will discuss follow-up recommendations based on your individual skin and treatment history.
